 While peripheral nerve blocks with local anesthetic medications may result in motor weakness, Ilfeld and colleagues suggest that peripheral nerve stimulation may avoid this “undesirable” effect. Peripheral nerve stimulators can also provide pain relief for patients with chronic neuropathic pain who have contraindications to spinal cord stimulator placement and provide lasting relief without adverse effects of pain medications. The use of peripheral nerve stimulators can provide regional anesthesia without systemic effects common with most pain medications. The concept of replacing opioids for this type of pain management holds promise in light of the current opioid crisis in America. Some studies suggest that peripheral nerve stimulators can successfully treat post-operative and acute pain with minimal need for opioid pain medications. Placement of peripheral nerve stimulators for analgesia could significantly change practice patterns for health care providers and could substantially impact patient satisfaction and quality of life. Upon confirmation of placement, the lead is secured in place with a sterile dressing. Appropriate placement results in comfortable sensations in the desired region without muscle contraction via the electrical stimulation. Once the needle is withdrawn, the lead can be attached to a stimulator, and a surface electrode is placed on the ipsilateral limb. The needle is then removed over the stimulator lead. The monopolar needle then gets withdrawn and the introducer needle pre-loaded with the stimulator lead is placed in the same location. Readjustment of the stimulator needle continues until muscle contractions and discomfort are no longer present. Inducing uncomfortable local sensations is associated with superficial needle placement, and distal discomfort or muscle contractions are associated with too deep of needle placement. An electrical stimulator is attached to the needle to deliver a test stimulation. A monopolar needle is inserted under ultrasound guidance up to 0.5cm to 1cm from the target nerve. A skin wheal is raised to ensure adequate cutaneous anesthesia. The provision of anesthesia to the insertion site is by injecting a local anesthetic under ultrasound guidance along the track of proposed needle insertion. The procedure requires the use of sterile gloves, surgical cap, and mask at a minimum and skin prep with chlorhexidine is recommended - and placement of a sterile dressing over the lead to maintain its position is also standard procedure. A machine for delivering electrical stimulation is necessary for testing the lead and providing continuous stimulation. 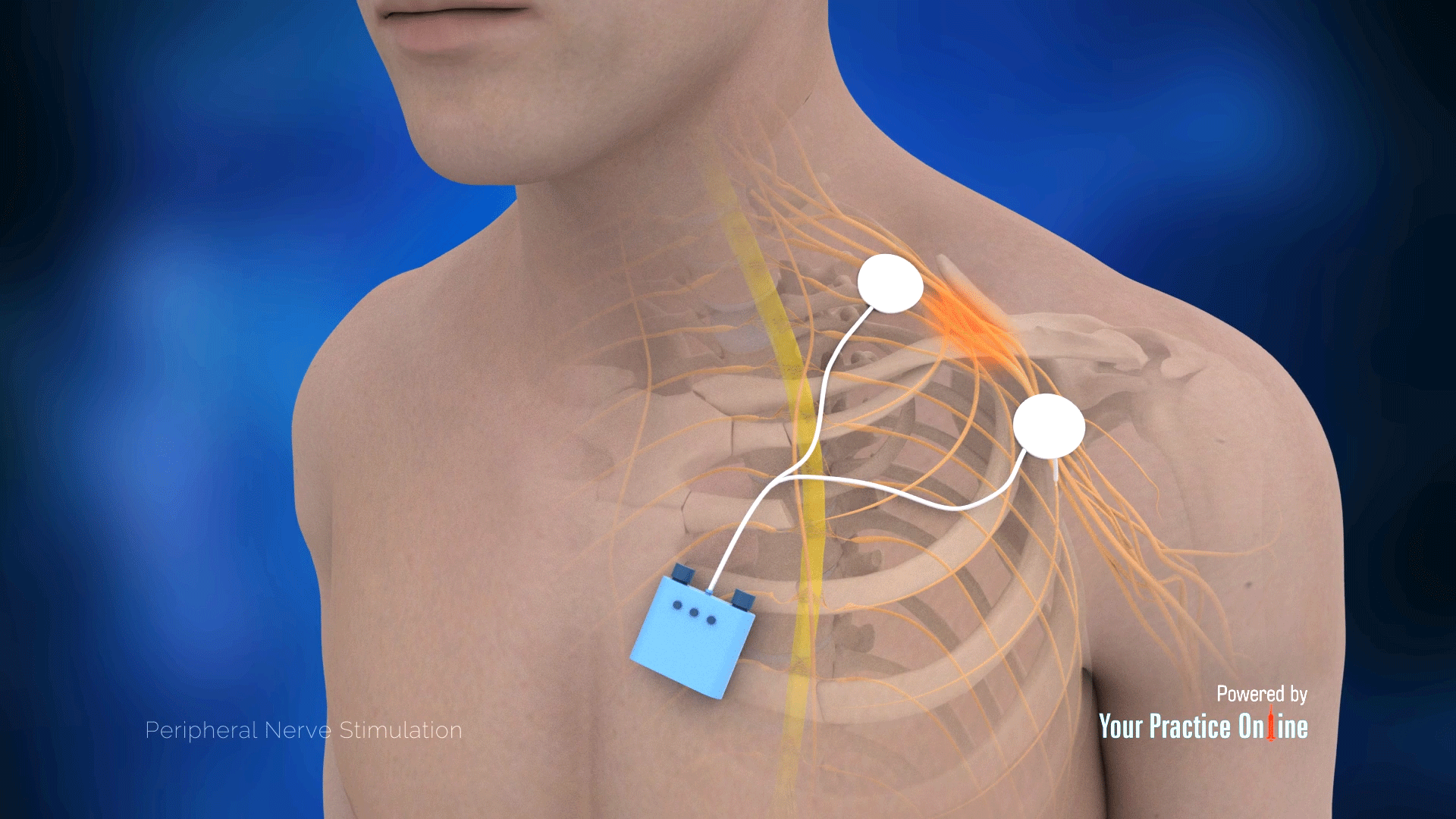
An introducer needle and stimulator lead serve to place the peripheral nerve stimulator. A monopolar needle electrode for testing optimal lead placement is also recommended. A small volume of local anesthetic for skin anesthesia is the recommended procedure. A sterile transducer sleeve should be utilized for this procedure as well. Any ultrasound machine with either a curved array transducer or linear array transducer may be used.   
Necessary equipment for placing a peripheral nerve stimulator include ultrasound for identification of target nerve, equipment to maintain sterility of the procedure, appropriate needles for monopolar lead placement, and a sterile dressing. The uses of peripheral nerve stimulators have not yet been fully explored, but several studies suggest that this technique is a feasible adjunct to current pain management practices. In addition, post-operative pain control may be achievable using peripheral nerve stimulation. Previously percutaneous peripheral nerve stimulators have been used for chronic neuropathic pain in patients with contraindications to spinal cord stimulators, and permanent lead placement has been the choice for chronic neuropathic pain. In this changing setting, peripheral nerve stimulators may serve as an important adjunct in both chronic and acute pain management. Managing chronic pain continues to be a challenge secondary to increasing opioid-related deaths and the opioid crisis. Non-opioid analgesia is a growing field and is gaining increased traction among pain physicians. Chronic pain is one of the leading causes of disability in the world. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
